- How Blue Light Impacts Your Sleep Quality
- Comparing Whey and Plant-Based Protein: Which is Best?
- How Long Does Nicotine Remain in Your System?
- The Best Time of Day to Drink Bone Broth to Maximize Health Benefits
- 8 Ways to Increase Dopamine Naturally
- 7 Best Breads for Maintaining Stable Blood Sugar
- Gelatin vs. Collagen: Which is Best for Skin, Nails, and Joints?
- The Long-Term Effects of Daily Turmeric Supplements on Liver Health
- Could Your Grocery Store Meat Be Causing Recurring UTIs?
- Are You Making This Expensive Thermostat Error This Winter?
Osteoporosis Drugs Work, But Review Finds No Clear Winner

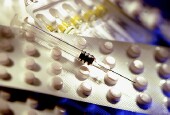
Many osteoporosis drugs cut women’s risk of suffering a bone fracture, though it’s not clear whether any one medication works better than others, a new research review finds.
Reporting Sept. 8 in Annals of Internal Medicine, researchers said that for women with the bone-thinning disease osteoporosis, various drugs cut the risk of a spine fracture by 40 to 60 percent, compared to a placebo.
When it comes to other bone breaks, including hip fractures, the drugs lower the risk by 20 to 40 percent, the study said.
The beneficial drugs included bisphosphonates, sold under brand names such as Actonel (risedronate), Boniva (ibandronate) and Fosamax (alendronate), and the injection drugs denosumab (Prolia) and teriparatide (Forteo).
Meanwhile, raloxifene (Evista) — a daily pill that has estrogen-like effects on bones — seems to cut the risk of spine fractures only, the study authors said.
There are still important unknowns, the researchers say.
It’s not clear, for example, which medications work best. “There’ve been very few head-to-head comparison studies,” said Dr. Carolyn Crandall, a professor of medicine at the University of California, Los Angeles, who led the review.
And most evidence of benefit is for women with full-blown osteoporosis or a previous fracture, Crandall said.
“There’s much less data on men, and on women with osteopenia,” she said. Osteopenia refers to lower-than-normal bone density that is not yet in the osteoporosis range.
In the United States, about 52 million people have low bone mass or outright osteoporosis, according to the National Osteoporosis Foundation. And among women older than 50, it’s estimated that half will suffer a fracture because of thinning bones.
The risks of osteoporosis drugs have gotten a lot of media attention of late. Bisphosphonates, for example, are linked to “atypical” fractures of the thigh bone and osteonecrosis of the jaw — where bone tissue in the jaw begins to die.
Crandall said the new findings help put the risks in perspective.
“These problems are rare,” she said. “Knowing the numbers might help the public, so they don’t get misled.”
Across studies of bisphosphonates, atypical thigh fractures happened in anywhere from two to 100 women for every 100,000 using the drugs, Crandall’s team found. The rate of jaw osteonecrosis ranged widely across studies — from 0.03 percent to 4 percent — but overall, the side effect does appear rare, Crandall said.
It’s not only rare, but also most often seen in cancer patients on high-dose IV bisphosphonates, said Dr. Robert Recker, who directs the Osteoporosis Research Center at Creighton University in Omaha, Neb.
“The benefits for most people with osteoporosis far outweigh the risks,” said Recker, who wasn’t involved in the study. “There’s broad consensus that they lower the risk of fracture.”
The more common side effects of bisphosphonates — heartburn, muscle pain and throat irritation — aren’t serious. But some people find them hard to tolerate, Recker said, and might need a different medication.
The two injection drugs, denosumab and teriparatide, are approved for women and men at high risk of a fracture. Denosumab, which blocks the cells that break bones down, can lower blood calcium levels and cause infections, including bladder and skin infections.
Teriparatide, which helps trigger bone formation, is self-injected every day, for up to two years. It can cause headaches, leg cramps and joint pain, and raise blood calcium levels.
The daily pill raloxifene can cause hot flashes and blood clots in a very small percentage of women, Crandall’s team found.
Often, Recker said, a patient’s choice of osteoporosis drug comes down to things like convenience. Denosumab has to be injected by a doctor — but only twice a year. “Some people like that,” Recker noted.
But an even bigger factor, he said, is cost.
Bisphosphonates have inexpensive generic versions, and they’re the usual first-choice osteoporosis treatment. In contrast, raloxifene and denosumab can cost more than $200 a month, while teriparatide tops $1,000 a month.
Crandall said the “optimal duration” of treatment, with any of the drugs, is still unclear.
“A lot of patients and doctors want to know if there’s a point where you can stop treatment and still get the benefit,” she said. “Unfortunately, we don’t have good evidence on that yet.”
The review included 294 studies published between 2005 and March 2014. It was funded by the U.S. Agency for Healthcare Research and Quality, and the RAND Corporation, a nonprofit research institute.
More information
The U.S. Agency for Healthcare Research and Quality has more on choosing an osteoporosis treatment.
Source: HealthDay
Copyright © 2026 HealthDay. All rights reserved.










