- How Blue Light Impacts Your Sleep Quality
- Comparing Whey and Plant-Based Protein: Which is Best?
- How Long Does Nicotine Remain in Your System?
- The Best Time of Day to Drink Bone Broth to Maximize Health Benefits
- 8 Ways to Increase Dopamine Naturally
- 7 Best Breads for Maintaining Stable Blood Sugar
- Gelatin vs. Collagen: Which is Best for Skin, Nails, and Joints?
- The Long-Term Effects of Daily Turmeric Supplements on Liver Health
- Could Your Grocery Store Meat Be Causing Recurring UTIs?
- Are You Making This Expensive Thermostat Error This Winter?
Surgery Can Boost Outcomes After Chemo for People With Pancreatic Cancer
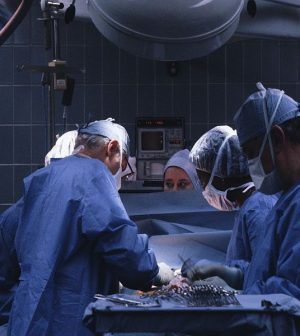
Even in patients with stage 2 pancreatic cancer, surgery is typically worthwhile after chemotherapy, because it appears to extend patients’ lives, a new study concludes.
In stage 2 cancer, the tumor has already grown large enough to be close to vessels that supply blood to nearby organs, such as the liver or intestines.
That can complicate surgeries and cause doctors to hesitate going forward with tumor-removing procedures, explained a team led by surgical oncologist Dr. Amanda Arrington, of the University of Arizona, Tucson.
However, based on her team’s analysis of almost 12,000 stage 2 pancreatic cancer patients, “surgeons can be a little more aggressive and offer surgical treatment more often than not,” Arrington said in a news release from the Journal of the American College of Surgeons. Her team published its findings in the journal on March 26.
One expert who wasn’t involved in the report called it a potential win for people with pancreatic cancer, which is so often fatal.
“Everyone with localized (non-metastatic) pancreatic cancer should be referred to a surgeon with expertise in pancreatic cancer,” said Dr. Danielle DePeralta, a surgical oncologist at Northwell Health Cancer Institute, in Lake Success, N.Y. “This allows for a nuanced discussion about whether that person’s tumor is amenable to resection.”
She hopes that results like those in the new study will bolster efforts to get more patients who could benefit into surgery.
“Surgery is mandatory to achieve cure,” DePeralta said, but “some physicians still see pancreatic cancer as a death sentence and think surgery is too risky. This type of thinking is outdated. Improvements in surgical technique and chemotherapy have allowed many patients to achieve a cure and maintain excellent quality of life after surgery.”
In the new study, Arrington’s group used a major U.S. database to track outcomes for almost 12,000 patients diagnosed and treated for stage 2 pancreatic cancer between 2010 and 2015.
About 81% were treated with tumor-shrinking chemotherapy alone, while about 19% got chemo plus surgery. Among those who got surgery, about 84% got it as their first-line treatment, while about 16% got chemotherapy that was then followed by surgery.
Patients who underwent surgery typically had “positive margins,” meaning stray cancer cells were detected in tissues near the site of the removed tumor.
A combination of chemotherapy plus surgery was tied to better survival. For example, patients who only got chemo survived an average of 10.2 months; those who got surgery before their chemo survived close to 18 months; and those who got chemotherapy first and surgery after survived an average of almost 20 months, the investigators found.
Their conclusion: Surgery after chemotherapy can be of real benefit to stage 2 pancreatic cancer patients, even when margins are positive for residual cancer. “There are ongoing studies looking at whether more pancreatic cancer patients, including stage 1 patients, would benefit from surgery after chemotherapy,” Arrington said.
For her part, DePeralta stressed that outcomes for pancreatic cancer patients are increasingly less hopeless as treatments continue to improve.
“For the first time, in 2020, five-year survival hit double digits at 10%. This includes patients of all stages,” she said. “Patients with stage 4 disease have pancreatic cancers that have spread, or metastasized, to other organs. Alex Trebek and Patrick Swayze are well known examples of people who died from stage 4 pancreatic cancer.”
The outlook is more promising for people spotted with earlier-stage disease. For patients with stage 1, 2 or (sometimes) 3 pancreatic tumors, many “can be cured with a combination of chemotherapy, surgery, and sometimes radiation,” DePeralta said.
“In cases where I am worried that the tumor is adherent to major blood vessels or other key structures, I recommend the patient receive two to four months of chemotherapy and radiation before trying to remove the tumor in the operating room,” she advised. “This minimizes the chances of leaving any tumor behind and increases the likelihood of cure.”
More information
There’s much more on pancreatic cancer and its treatment at the Pancreatic Cancer Action Network.
SOURCES: Danielle DePeralta, MD, surgical oncologist, Northwell Health Cancer Institute, Lake Success, N.Y.; Journal of the American College of Surgeons, news release, March 26, 2021
Source: HealthDay
Copyright © 2026 HealthDay. All rights reserved.










