- How Blue Light Impacts Your Sleep Quality
- Comparing Whey and Plant-Based Protein: Which is Best?
- How Long Does Nicotine Remain in Your System?
- The Best Time of Day to Drink Bone Broth to Maximize Health Benefits
- 8 Ways to Increase Dopamine Naturally
- 7 Best Breads for Maintaining Stable Blood Sugar
- Gelatin vs. Collagen: Which is Best for Skin, Nails, and Joints?
- The Long-Term Effects of Daily Turmeric Supplements on Liver Health
- Could Your Grocery Store Meat Be Causing Recurring UTIs?
- Are You Making This Expensive Thermostat Error This Winter?
If Protections Expire, COVID Patients Could Soon Face Big Medical Bills
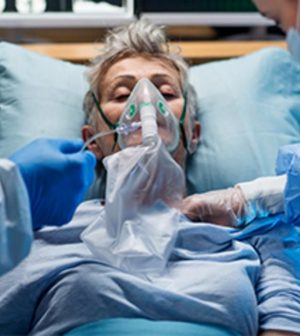
Older Americans on a Medicare Advantage plan could face hospital bills of $1,000 or more if private insurers start charging out-of-pocket costs for lifesaving COVID-19 care, a new study warns.
Cost data show that Medicare Advantage patients pay an average $987 out-of-pocket when they are hospitalized with the seasonal flu, and about 3% pay more than $2,500, according to the report.
To put that in perspective, two of every five Americans lack the savings to pay for even a $400 emergency, the researchers noted.
So far, nearly all private insurance companies have volunteered to provide full coverage for all expenses from COVID-19-related hospital stays.
But billing related to flu hospitalizations provides a good notion of what might await seniors treated for severe COVID-19 if insurers decide to change their minds and start charging out-of-pocket costs, said lead researcher Dr. Kao-Ping Chua. He’s an assistant professor with the University of Michigan Medical School, in Ann Arbor.
Influenza “predominantly affects the elderly and often requires a lot of the same types of care,” Chua said. “It’s the closest analogue we have.”
Nearly 1.7 million COVID-19 hospitalizations have occurred during the past year, and the coronavirus tends to hit older people harder than other groups, the researchers said in background notes.
Matthew Eisenberg is an assistant professor of health policy and management with the Johns Hopkins Bloomberg School of Public Health, in Baltimore. He said, “Now that we more firmly know that most of the hospitalizations are focused in the over-65 population, understanding the cost that the Medicare Advantage population may have to pay is quite important.”
About one-third of U.S. seniors subscribe to Medicare Advantage rather than traditional Medicare, according to the Kaiser Family Foundation. These plans provide Medicare benefits through a private-sector health insurer.
There’s no federal legislation requiring health insurers to waive COVID-19 treatment costs, Chua noted. Instead, the insurance companies have chosen on their own to waive cost-sharing for COVID-19 hospitalizations, but it’s not clear how long those waivers will remain in place.
“Recently, some of the insurers have begun to walk back some of those waivers, raising the possibility that patients who are hospitalized for COVID-19 might not just have to deal with the physical and emotional toll, but also face a financial dilemma afterwards,” Chua said.
To get some idea of the potential cost to older Americans if these waivers end, Chua and his colleagues analyzed data from more than 14,000 influenza hospitalizations covered by Medicare Advantage in 2018. Their findings were published online Feb. 17 in the American Journal of Preventive Medicine.
Flu patients faced higher cost-sharing expenses if they needed intensive care or had a long hospital stay, both of which are common for severe COVID-19 patients, the researchers noted. People also paid more if they were enrolled in a preferred provider organization (PPO) plan versus an HMO.
Federal regulators should keep these costs in mind as insurance companies start to rethink their position on COVID-19 care waivers, Chua and Eisenberg said.
The U.S. Centers for Medicare and Medicaid Services might be able to unilaterally require insurers to maintain these waivers, Eisenberg said.
“When it comes to Medicare Advantage plans, the government has quite a bit of say in how these plans operate,” Eisenberg said. “I am not entirely sure if the administration could waive this unilaterally and require Medicare Advantage plans to not charge any cost-sharing for COVID care. I think the administration could do this unilaterally, but I’m not 100% sure.”
If that’s not possible, Chua said, Congress should consider stepping in with legislation that would mandate cost-sharing waivers for COVID-19 care.
Earlier legislation related to COVID-19 has contained similar provisions, though none have been enacted, Chua said.
“It’s not like this is a pipe dream. This is an issue that federal policy makers understand, and there certainly is some appetite in at least some quarters to act to protect patients,” he added.
In the meantime, seniors should check their Medicare Advantage plan to make sure that COVID-19 costs are still waived, and appeal any charges that they don’t think are warranted, Chua said.
COVID-19 patients can also ask the hospital to waive expenses as charity care or set up a billing plan to spread out the cost, although Chua admitted these are “imperfect” remedies when facing a huge medical bill.
More information
America’s Health Insurance Plans maintains a list of individual private insurers’ waivers related to COVID-19 care.
SOURCES: Kao-Ping Chua, MD, PhD, assistant professor, University of Michigan Medical School, Ann Arbor; Matthew Eisenberg, PhD, assistant professor, health policy and management, Johns Hopkins Bloomberg School of Public Health, Baltimore; American Journal of Preventive Medicine, Feb. 17, 2021, online
Source: HealthDay
Copyright © 2026 HealthDay. All rights reserved.










