- How Blue Light Impacts Your Sleep Quality
- Comparing Whey and Plant-Based Protein: Which is Best?
- How Long Does Nicotine Remain in Your System?
- The Best Time of Day to Drink Bone Broth to Maximize Health Benefits
- 8 Ways to Increase Dopamine Naturally
- 7 Best Breads for Maintaining Stable Blood Sugar
- Gelatin vs. Collagen: Which is Best for Skin, Nails, and Joints?
- The Long-Term Effects of Daily Turmeric Supplements on Liver Health
- Could Your Grocery Store Meat Be Causing Recurring UTIs?
- Are You Making This Expensive Thermostat Error This Winter?
Out-of-Pocket Medical Bills for COVID-19 May Average $3,800 in 2021: Study
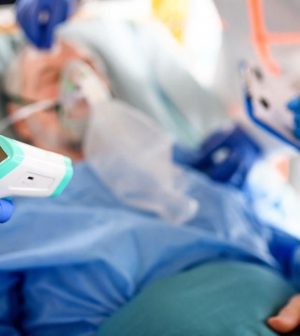
Americans hospitalized with COVID-19 could now face thousands of dollars in out-of-pocket medical costs, according to a new report.
In 2020, most health insurance companies waived co-pays, deductibles and other cost-sharing for hospitalized COVID-19 patients, but many stopped doing that early this year, the University of Michigan researchers noted.
“Many insurers claim that it is justified to charge patients for COVID-19 hospitalizations now that COVID-19 vaccines are widely available,” said study lead author Dr. Kao-Ping Chua, a health policy researcher and pediatrician at Michigan Medicine, in Ann Arbor.
“However, some people hospitalized for COVID-19 aren’t eligible for vaccines, such as young children, while others are vaccinated patients who experienced a severe breakthrough infection. Our study suggests these patients could [have] substantial bills,” Chua said in a university news release.
For this study, the researchers analyzed data from more than 4,000 COVID-19 hospitalizations of people with private insurance and Medicare Advantage insurance between March and September 2020.
The vast majority of patients didn’t have to pay for hospital services, suggesting their plans waived cost-sharing for bills sent by hospitals.
But the few patients who did have to pay for hospital services — an indication that a waiver wasn’t in place — had out-of-pocket costs in the thousands of dollars.
Based on last year’s information, the researchers said hospitalized COVID-19 patients without waivers could now face out-of-pocket bills of about $3,800 for those with private insurance, and $1,500 for those with Medicare Advantage plans.
The findings could have implications for people who haven’t been vaccinated and those with underlying conditions that put them at risk of a severe breakthrough case of COVID-19, according to the authors. The results were published online Oct. 18 in JAMA Network Open.
The researchers also found that insurer cost-sharing waivers for COVID-19 hospitalizations don’t always cover all hospitalization-related care. For example, many patients in the study received bills from doctors who cared for them in the hospital and from ambulance companies.
Overall, 71% of privately insured patients received a bill for any hospitalization-related service, with an average cost of $788. Among those with Medicare Advantage coverage, about half received a bill, with an average cost of $277.
Chua said he’s concerned that “the threat of high costs might cause some patients with severe COVID-19 to delay going to the hospital, increasing their risk of death.”
He said the federal government should require insurers to waive costs of COVID-19 hospitalization-related care throughout the pandemic, as they do for COVID-19 testing and vaccination.
However, that’s unlikely to happen given widespread anger against the unvaccinated, Chua said.
More information
The U.S. Department of Health and Human Services outlines COVID-19 treatments.
SOURCE: University of Michigan, news release, Oct. 18, 2021
Source: HealthDay
Copyright © 2026 HealthDay. All rights reserved.










