- How Blue Light Impacts Your Sleep Quality
- Comparing Whey and Plant-Based Protein: Which is Best?
- How Long Does Nicotine Remain in Your System?
- The Best Time of Day to Drink Bone Broth to Maximize Health Benefits
- 8 Ways to Increase Dopamine Naturally
- 7 Best Breads for Maintaining Stable Blood Sugar
- Gelatin vs. Collagen: Which is Best for Skin, Nails, and Joints?
- The Long-Term Effects of Daily Turmeric Supplements on Liver Health
- Could Your Grocery Store Meat Be Causing Recurring UTIs?
- Are You Making This Expensive Thermostat Error This Winter?
Could Threshold for COVID-19 Herd Immunity Be Lower Than Thought?
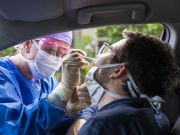
Could young people going out and partying be the key to limiting the spread of COVID-19?
Possibly, as a new mathematical model argues that herd immunity might be achieved with fewer people becoming immune through infection than was believed, if you take into account how the virus would spread among younger, more socially active folks.
The model estimates that herd immunity could occur after 43% of the population becomes immune to COVID-19 by passing the disease from person to person, far lower than the 60% to 70% figure that epidemiologists have held out as the gold standard.
This estimate is based on the argument that younger and more socially active people are the main spreaders of infectious disease, and therefore will contribute more to herd immunity after they’ve been infected and gotten over COVID-19, said lead researcher Tom Britton, a professor of mathematical statistics at Stockholm University in Sweden.
Traditional estimates for herd immunity are based on vaccination, and assume that everyone in a community is equally likely to achieve immunity by getting inoculated.
But those estimates are flawed because they don’t take into account the herd immunity achieved from a disease spreading through a community, Britton and his researchers argued.
“When immunity instead comes from having been infected, then immunity is more spread among the outgoing people exposing themselves and others to the disease more,” Britton continued. “This latter immunity is hence distributed in a more efficient manner, which in turn implies that fewer are needed to reach herd immunity.
“Immunity coming from disease exposure is spread more among more socially active people, which makes the effect stronger than the corresponding immunity level when performing vaccination,” Britton summed up.
However, there are some problems with the reasoning behind the model when it comes to COVID-19, infectious disease experts note.
For one thing, scientists don’t yet know whether a cured COVID-19 patient will be immune from the virus for an extended period, said Dr. Waleed Javaid, director of infection prevention and control at Mount Sinai Downtown in New York City.
It’s also not yet known whether the COVID-19 coronavirus will be able to mutate in ways that get around a person’s immunity, he added.
“We’ll probably see a lot more models like this, but I think more practically we’ll have to wait a year or more to see studies that are actual,” based on hard data about human immunity to COVID-19, Javaid said.
The model offers a good argument that “if there is a certain segment of the population that is less likely to get infected naturally versus those who are more likely to get infected, this may alter the herd immunity threshold,” said Dr. Amesh Adalja, a senior scholar with the Johns Hopkins Center for Health Security.
But the model doesn’t take into account the effect on the health care system if a huge number of young partygoers become infected at the same time, Adalja added.
“Natural herd immunity with a virus like this is going to be hard to achieve without placing an enormous burden on hospitals, but the paper is a useful thought experiment that improves the way we think about the concept of herd immunity,” Adalja said.
It also would be “very selfish” for young, socially active people to go out and intentionally become infected with COVID-19, because of the potentially dire consequences to others in their lives, Javaid said.
“If I’m young and I get it, I might get over it, but the people I contact, if any of them are older, they might die because of the contact I had with them after I got the illness,” Javaid said, noting that the elderly and immune-compromised are much more likely to have a fatal case of COVID-19.
However, the researchers said their model does support the gradual lifting of lockdown restrictions related to COVID-19, so that hospitals do not become overwhelmed even as people are infected and gain immunity.
“The paper is not an argument to aim for herd immunity,” Britton said. “The result of the paper just says that herd immunity happens with fewer infected, and also that the effect of immunity when herd immunity is not reached is stronger than initially believed.”
The finding was published recently in the journal Science.
More information
The Johns Hopkins Bloomberg School of Public Health has more about COVID-19 and herd immunity.
Source: HealthDay
Copyright © 2026 HealthDay. All rights reserved.










