- How Blue Light Impacts Your Sleep Quality
- Comparing Whey and Plant-Based Protein: Which is Best?
- How Long Does Nicotine Remain in Your System?
- The Best Time of Day to Drink Bone Broth to Maximize Health Benefits
- 8 Ways to Increase Dopamine Naturally
- 7 Best Breads for Maintaining Stable Blood Sugar
- Gelatin vs. Collagen: Which is Best for Skin, Nails, and Joints?
- The Long-Term Effects of Daily Turmeric Supplements on Liver Health
- Could Your Grocery Store Meat Be Causing Recurring UTIs?
- Are You Making This Expensive Thermostat Error This Winter?
Even at Cancer Centers, Finding Relief for Pain Can Be Tough
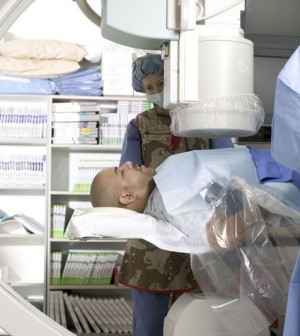
Staff members at nearly one in 10 major U.S. cancer centers — all of which provide palliative care services — weren’t certain such symptom-management and supportive care was actually available there, a new study reveals.
The study suggests that for cancer patients, obtaining good relief for their stress and pain may not always be easy, the researchers said.
Using an undercover “mystery shopper” approach, the Duke University team also had difficulty getting information about palliative care services during about one-third of calls to 40 U.S. National Cancer Institute-designated cancer centers.
“We were surprised that when we did get in touch with people [at these centers], so frequently we weren’t able to get these questions answered,” said study author Kathryn Hutchins, a fourth-year medical student at Duke, in Durham, N.C.
She said part of the problem accessing palliative care, even at hospitals incorporating it, stems from widespread confusion about the differences between palliative care and hospice care.
Palliative care aims to control symptoms, side effects and stress throughout illness regardless of prognosis, while hospice care is offered only at end-of-life stages.
The study was presented earlier this month at a meeting of the American Society of Clinical Oncology (ASCO) in San Francisco. Research presented at scientific conferences typically hasn’t been peer-reviewed or published, and results are considered preliminary.
In the study, Hutchins and her team used a “mystery shopper” approach — making 160 phone calls to 40 cancer centers on different days, asking about palliative and supportive care needs for a fictitious family member recently diagnosed with inoperable liver cancer.
In nearly 10 percent of calls, staff members gave an answer other than “yes” when asked about the availability of palliative care services there, even though such services were indeed available.
While answers varied, responses included inaccurate statements such as that palliative care was only for end-of-life patients; that no physicians there specialized in symptom management; or that a medical record review would be needed first.
In other responses, the person answering the phone was unsure of either the availability of palliative care or didn’t know what the term meant, the study found.
Only about 38 percent of callers were correctly told that all seven supportive care services they asked about were offered at the cancer center.
The “mystery shopper” format “just seemed like the most genuine way to get answers to those questions,” Hutchins said.
“This kind of research speaks to the idea that when calling a major cancer center, there are people who … have the same misconceptions [as the public] about palliative care,” she added. “The people we spoke to were warm and kind, but they didn’t have the information we needed.”
Hutchins and another expert both believe that high staff turnover at cancer centers may add to the problem.
“With different people serving in this role, it may not necessarily be part of their training to make sure they’re well-versed in what the cancer center offers,” Hutchins said.
Dr. Andrew Epstein, an ASCO spokesman for palliative care, agreed, saying, “The devil is in the details as to how much the people in those centers are aware of those services.”
Epstein, who wasn’t involved in the new research, felt the study’s undercover approach was particularly effective at revealing information gaps among staff members at cancer centers.
“While seeming sneaky at first … I think it provides an innovative and real-world, in-the-weeds example of what’s going on when the rubber meets the road,” said Epstein, a medical oncologist specializing in gastrointestinal cancers at Memorial Sloan Kettering Cancer Center in New York City.
Hutchins and Epstein agreed that efforts to uniformly educate cancer center staff members are needed, along with public awareness campaigns about the true nature of palliative care services.
“We see there continues to be, even on the medical side, the misunderstanding about what palliative care is,” Epstein said.
More information
There’s more on palliative care at the U.S. National Cancer Institute.
Source: HealthDay
Copyright © 2026 HealthDay. All rights reserved.










