- How Blue Light Impacts Your Sleep Quality
- Comparing Whey and Plant-Based Protein: Which is Best?
- How Long Does Nicotine Remain in Your System?
- The Best Time of Day to Drink Bone Broth to Maximize Health Benefits
- 8 Ways to Increase Dopamine Naturally
- 7 Best Breads for Maintaining Stable Blood Sugar
- Gelatin vs. Collagen: Which is Best for Skin, Nails, and Joints?
- The Long-Term Effects of Daily Turmeric Supplements on Liver Health
- Could Your Grocery Store Meat Be Causing Recurring UTIs?
- Are You Making This Expensive Thermostat Error This Winter?
How Do Americans Die? New Study Looks at Last Few Years of Life
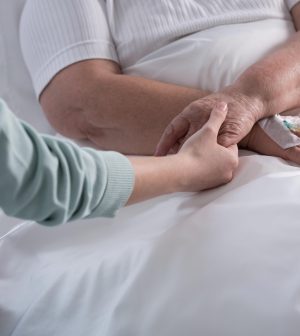
A sampling of the last three years of life spent by people who died in 2018 is giving a picture of what dying looks like in the United States.
The analysis was conducted by a team at Rutgers University in New Jersey. Researchers tracked the end-of-life “trajectories” of about 200,000 Medicare beneficiaries who died in 2018.
They found that about 6 in every 10 (59%) people spent the last three years of their lives at home, cared for by family and friends when they needed help with daily tasks.
Most of these people didn’t require professional care, or if they did it was only within the last year of life, the researchers noted.
Another 27% of people who died in 2018 fell into the “skilled home care” category. That means that they remained at home during the last three years of their lives but had skilled professionals, such as nurses, help with their care.
A smaller group (14%) required “institutional care.” These people spent the last three years of life in a nursing home or hospital, and got nearly all their care from paid professionals, the study found.
“Most people want to stay at home with minimal professional help,” said study senior author Olga Jarrín, a professor of nursing research at Rutgers. “However, the goal for a significant minority of people is to avoid being a burden to family and friends, and such people tend to want professional care.”
The study, published Jan. 24 in the journal BMC Geriatrics, also noted demographic patterns. For example, people who required some form of professional care (whether inside the home or in a nursing home) were more likely to be female than male. They were also more likely to be Black than white and to be on Medicaid, Jarrin’s group found.
That might reflect “clinical and policy factors that dictate where and when patients receive care,” said lead study author Haiqun Lin, a professor of biostatistics at Rutgers.
“Understanding these patterns is crucial for advance care planning,” Lin added in a Rutgers news release.
Jarrin agreed, saying the research is aimed at “designing interventions that send more people down whatever path is right for them.”
More information
Find out about advance care planning at the National Institute on Aging.
SOURCE: Rutgers University, news release, Jan. 24, 2024
Source: HealthDay
Copyright © 2026 HealthDay. All rights reserved.










