- How Blue Light Impacts Your Sleep Quality
- Comparing Whey and Plant-Based Protein: Which is Best?
- How Long Does Nicotine Remain in Your System?
- The Best Time of Day to Drink Bone Broth to Maximize Health Benefits
- 8 Ways to Increase Dopamine Naturally
- 7 Best Breads for Maintaining Stable Blood Sugar
- Gelatin vs. Collagen: Which is Best for Skin, Nails, and Joints?
- The Long-Term Effects of Daily Turmeric Supplements on Liver Health
- Could Your Grocery Store Meat Be Causing Recurring UTIs?
- Are You Making This Expensive Thermostat Error This Winter?
New Approach to Transplants Could Boost Supply of Donor Hearts
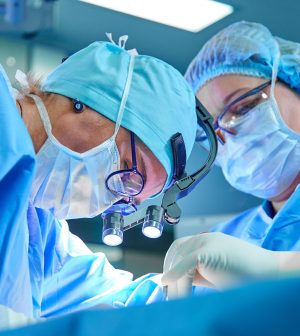
A new transplant method that “reanimates” donor hearts appears safe and effective, a new clinical trial has found — in an advance that could substantially expand the supply of donor hearts available in the United States.
The trial tested an approach that allows doctors to transplant hearts from donors who have succumbed to “circulatory death” — meaning the heart has stopped beating. Traditionally, heart transplants could only be done with a heart from a donor on life support who has been declared brain dead. That means all brain functions have ceased, but the heart and other organs are being maintained by machines.
But thanks to a new “heart-in-a-box” device, doctors can now take a donor heart that has stopped beating and essentially revive it, and test its function to determine if it’s suitable for transplant.
In the new trial, conducted at 15 U.S. transplant centers, doctors found that the approach was on par with traditional heart transplants.
Of 80 patients who received a reanimated donor heart, 94% were alive six months later. That compared with 90% of 86 patients who received hearts from brain-dead donors.
Experts said the results, published June 8 in the New England Journal of Medicine, are “exciting.”
The transplant approach, known as donation after circulatory death (DCD), could expand the national supply of donor hearts by about 30%, said lead researcher Dr. Jacob Schroder, surgical director of the heart transplant program at Duke University, in Durham, N.C.
“That’s still not enough,” Schroder said. “But I’d say this is the biggest thing to happen in heart transplantation since heart transplantation.”
DCD hearts come from donors who have suffered devastating injuries that have left them on life support with no chance of recovery. In most cases, they have severe brain injuries that fall short of the strict criteria used to declare brain death. Instead, they succumb to “circulatory death” after the family decides to withdraw life support.
In the United States, DCD transplants have long been done with other organs, including the kidneys, liver and lungs. Those organs, particularly the kidneys, can tolerate a period of oxygen deprivation after circulatory death. The heart, which has stopped beating in cases of circulatory death, has been the exception.
“For the longest time,” Schroder explained, “we didn’t have the methods to preserve and reanimate the heart.”
But in recent years, with the emergence of the new technology, transplant centers in some other countries have been using DCD hearts. Small studies in Australia and the United Kingdom have indicated that transplant recipients fare just as well with DCD hearts as they do with conventional transplants.
The new trial is the first to test the approach in the United States, using the Organ Care System made by TransMedics, a Massachusetts-based medical device company that funded the study. It’s a “heart-in-a-box” device that perfuses the donor heart with warm, oxygenated blood. In addition to resuscitating the heart, the device also allows doctors to test its function.
The trial enrolled 180 adult heart transplant candidates, with half receiving a DCD heart and half receiving one from a brain-dead donor.
At the six-month mark, the researchers analyzed the outcomes of 166 transplant recipients. Overall, survival rates were comparable between the two groups, as was the risk of serious problems with the new heart.
Patients in the DCD group were more likely to have significant heart-function issues soon after the transplant: 15% did, versus 5% in the standard transplant group. But the problems were manageable.
Right now, about 20 U.S. transplant centers perform DCD heart transplants, according to Schroder. But he said he thinks they should now be considered “a standard of care.”
Other experts expected the findings will encourage more transplant programs to adopt the approach.
The heart transplant field is, by nature, “very conservative,” said Dr. Nancy Sweitzer, a heart failure specialist and professor at Washington University School of Medicine in St. Louis.
Transplant teams want to be sure they’re “making a good trade” when they give patients a new heart, Sweitzer said.
“I do think these findings will lead more programs to go forward with this more confidently,” said Sweitzer, who wrote an editorial published with the study.
Dr. David Klassen is chief medical officer of the United Network for Organ Sharing (UNOS), the nonprofit that manages the national transplant waiting list. He said that compared with other organ transplants, heart transplants have always been more limited by donor supply.
According to Klassen, the new findings confirm what everyone has thought would be the case. But having solid data from a clinical trial is important, he said, to bolster programs’ confidence in DCD heart transplants.
Schroder said he believes it’s time to move away from the idea that heart transplants are limited by a “supply issue.” Instead, he thinks many programs can be less restrictive in what they deem a good donor heart.
In 2022, a record-high 4,111 heart transplants were performed in the United States, according to UNOS. Currently, there are 3,350 Americans on the wait list for a heart.
More information
The United Network for Organ Sharing has more on heart transplantation.
SOURCES: Jacob Schroder, MD, assistant professor, surgery, and surgical director, heart transplantation program, Duke University School of Medicine, Durham, N.C.; David Klassen, MD, chief medical officer, United Network for Organ Sharing, Richmond, Va.; Nancy Sweitzer, MD, PhD, professor, medicine, Washington University School of Medicine in St. Louis; New England Journal of Medicine, June 8, 2023
Source: HealthDay
Copyright © 2026 HealthDay. All rights reserved.










